Acupuncture for Depression: A TCM Approach to Mental Health
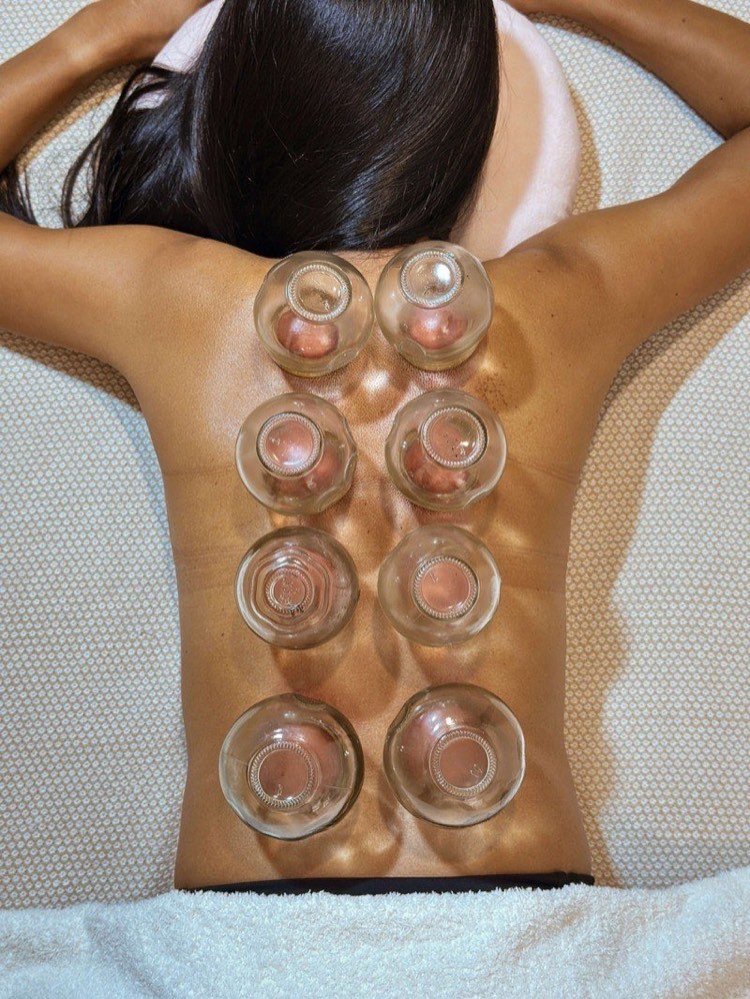
When the Light Goes Out
Depression does not always look like sadness. Sometimes it looks like numbness. A flatness where emotion used to be. The inability to enjoy things that once brought pleasure. A heaviness in the body that makes even simple tasks feel exhausting. A fog in the mind that makes decisions feel impossible. If this describes where you are right now, you are not broken. Your nervous system is stuck in a pattern, and acupuncture for depression can help shift it.
Traditional Chinese Medicine has been treating what we now call depression for over two thousand years. Long before the concept of serotonin or neurotransmitters existed, TCM practitioners identified distinct patterns of emotional disturbance and developed treatment protocols that restored balance. Modern research is now confirming what these practitioners observed clinically: acupuncture produces measurable changes in brain chemistry, nervous system function, and inflammatory markers that are directly relevant to depression.
How TCM Understands Depression
In TCM, depression is not a single disease with a single cause. It is an umbrella term for several distinct patterns, each with different characteristics and requiring different treatment approaches. This is one of the greatest strengths of the TCM approach: instead of prescribing the same treatment to every depressed patient, it identifies your specific pattern and treats accordingly.
Liver qi stagnation is the most common pattern associated with depression, particularly in its early stages. The Liver in TCM is responsible for the smooth flow of qi throughout the body and the free expression of emotions. When this flow is blocked, typically by chronic stress, frustration, suppressed anger, or a sense of being trapped in circumstances you cannot change, the result is emotional flatness, irritability that alternates with withdrawal, a feeling of tightness in the chest or throat, sighing, and mood that fluctuates unpredictably. You may not feel "sad" in the conventional sense but rather stuck, frustrated, and unable to feel anything fully.
Heart blood and Spleen qi deficiency produces a different presentation. This pattern develops when prolonged worry, overwork, poor diet, or chronic illness depletes the body's resources. The Heart in TCM houses the Shen (spirit or consciousness), and when Heart blood is insufficient, the Shen becomes unanchored. The result is persistent low mood, poor concentration, memory problems, fatigue, insomnia or disturbed sleep with vivid dreams, and a pale complexion. This pattern is common in people who have been under sustained pressure for months or years and have gradually run themselves empty. It often coincides with the kind of insomnia where you wake in the early hours with anxious, scattered thoughts.
Kidney yang deficiency produces what might be called the deepest form of depression in TCM. The Kidneys store the body's foundational energy, and when this energy is depleted, everything slows down. The result is profound fatigue, a cold heavy body, loss of motivation and drive, fear and anxiety, low libido, lower back pain, and a sense of existential depletion. This pattern is more common with aging, after major illness, after prolonged periods of extreme stress, or after grief. It is the TCM equivalent of burnout taken to its extreme.
Phlegm misting the Heart describes a pattern where mental clarity is obscured. The mind feels foggy, heavy, and dull. Decision making feels impossible. There may be a sensation of something blocking the throat (historically called "plum pit qi"). This pattern often develops from poor diet, excessive dampness (common in tropical climates), or long standing Spleen deficiency that fails to transform fluids properly. It can accompany or develop into a form of depression characterized more by apathy and mental heaviness than by sadness.
How Acupuncture Treats Depression
The mechanisms through which acupuncture affects depression are increasingly well understood by modern research, and they align closely with what TCM has described for centuries.
Neurotransmitter regulation. Acupuncture has been shown to increase levels of serotonin, norepinephrine, and dopamine, the same neurotransmitters targeted by antidepressant medications. It achieves this through stimulation of the hypothalamus and the modulation of the HPA (hypothalamic pituitary adrenal) axis. Unlike medication, which floods the system with a chemical override, acupuncture stimulates the body's own production pathways, which may explain why its effects tend to build gradually and persist after treatment ends.
Nervous system regulation. Depression is increasingly understood as a disorder of nervous system regulation. The autonomic nervous system becomes stuck in a pattern of either hyperarousal (anxiety, agitation, insomnia) or hypoarousal (numbness, fatigue, withdrawal). Acupuncture activates the vagus nerve and shifts the autonomic nervous system toward balance, helping the body move out of the stuck state. This is why many patients describe feeling "something shift" during or immediately after a session.
Inflammation reduction. A growing body of research links depression to chronic neuroinflammation. Elevated inflammatory markers (particularly IL-6, TNF-alpha, and CRP) are consistently found in depressed patients. Acupuncture has been shown to reduce these inflammatory markers, potentially addressing one of the root biological mechanisms of depression rather than just the symptoms.
HPA axis regulation. Chronic stress dysregulates the HPA axis, leading to elevated cortisol levels that damage brain structures involved in mood regulation (particularly the hippocampus and prefrontal cortex). Acupuncture normalizes cortisol rhythms, reducing the allostatic load on these brain structures and supporting their recovery.
Brain connectivity. Functional MRI studies have shown that acupuncture modulates activity in brain regions associated with emotional processing, including the amygdala, anterior cingulate cortex, and prefrontal cortex. These are the same regions that show altered function in depression and the same regions targeted by newer treatments like transcranial magnetic stimulation.
What the Research Says
A landmark meta analysis published in the Journal of Clinical Medicine in 2019, examining 64 randomized controlled trials with over 7,000 participants, concluded that acupuncture is effective for treating major depressive disorder. The analysis found that acupuncture produced significantly greater improvement compared to sham acupuncture, was as effective as antidepressant medication, and when combined with medication, produced better outcomes than medication alone.
A Cochrane review examining acupuncture for depression found moderate quality evidence that acupuncture reduces the severity of depression and that electroacupuncture may be particularly effective. The review noted that acupuncture had significantly fewer adverse effects than antidepressant medication.
Research published in the journal PLOS ONE demonstrated that acupuncture was as effective as fluoxetine (Prozac) for mild to moderate depression over an eight week treatment course, with the acupuncture group experiencing significantly fewer side effects.
These findings do not suggest that acupuncture should replace medication for everyone. Severe depression may require pharmaceutical intervention, and there is no shame in that. What the research does show is that acupuncture is a legitimate, evidence based treatment option that works through distinct biological mechanisms and can be used alone for mild to moderate depression or alongside medication for more severe cases.
Acupuncture and Antidepressants: Can They Work Together?
Yes. Acupuncture works safely alongside antidepressant medication and may enhance its effectiveness. Research consistently shows that patients receiving both acupuncture and medication improve more than those receiving medication alone. Acupuncture may also help reduce the side effects that cause many patients to discontinue their medication, including digestive issues, insomnia, weight gain, and sexual dysfunction.
If you are currently taking antidepressants and want to explore acupuncture as a complementary treatment, you should continue your medication and inform both your prescribing doctor and your acupuncturist. Never stop or reduce medication without medical guidance.
For some patients, acupuncture eventually supports a medically supervised tapering of medication. This is a conversation to have with your doctor once you have established a stable improvement pattern, not a goal to rush toward.
What Treatment at Piraluna Looks Like
When you come to Piraluna for depression, the first session involves a detailed assessment. Claire will ask about your emotional state, your energy patterns throughout the day, your sleep, your appetite, your physical symptoms, and the circumstances surrounding the onset of your depression. She examines your pulse and tongue to identify the TCM pattern driving your symptoms.
Treatment is then tailored to your specific pattern. Liver qi stagnation calls for points that move stuck energy and open the chest. Heart blood and Spleen qi deficiency requires nourishing, tonifying points that rebuild depleted resources. Kidney yang deficiency benefits from warming techniques including moxibustion. Phlegm misting the Heart needs points that resolve phlegm and clear the mind.
Sessions last approximately 60 minutes. The experience is deeply calming. Most patients feel a noticeable shift in their emotional state during or immediately after treatment, often described as a lifting of heaviness, a sense of opening in the chest, or simply feeling more present and alive.
For depression, Claire typically recommends weekly sessions for an initial course of eight to twelve weeks. Many patients notice improvement within the first three to four sessions, with changes building progressively. Some patients continue with less frequent maintenance sessions after the initial course.
Acupressure Points for Mood Support Between Sessions
These points can be pressed firmly for one to two minutes each, two to three times daily, to support your mood between acupuncture sessions. They are not a substitute for professional treatment but can help maintain momentum between visits.
Liver 3 (Taichong). On the top of the foot, in the depression between the first and second metatarsal bones, about two finger widths up from the web between the big toe and second toe. This is the primary point for moving Liver qi stagnation. Press firmly; it is often quite tender when qi is stuck. This point is excellent for the frustrated, stuck, emotionally flat presentation of depression.
Heart 7 (Shenmen). On the inner wrist crease, in the small depression on the pinky side of the tendon that runs down the center of the wrist. This point calms the Shen, nourishes Heart blood, and reduces anxiety. It is particularly helpful for the racing thoughts and insomnia that accompany depression. Press gently and breathe slowly while holding the point.
Pericardium 6 (Neiguan). Three finger widths above the inner wrist crease, between the two tendons. This point opens the chest, releases the feeling of emotional constriction, and has a powerful calming effect on the nervous system. If you feel tightness in your chest or a lump in your throat when emotions are suppressed, this point directly addresses that sensation.
Governing Vessel 20 (Baihui). On the top of the head, at the intersection of a line drawn from the tips of both ears over the crown. This point lifts yang energy upward, clears the mind, and is specifically indicated for depression with heaviness, foggy thinking, and sinking energy. Press gently and hold for one to two minutes, breathing deeply.
Beyond Acupuncture: Lifestyle Factors That Support Recovery
Acupuncture creates internal shifts, but your daily habits either support or undermine those shifts. A few things matter enormously.
Movement. Exercise is one of the most consistently effective interventions for depression across all research. It does not need to be intense. A 30 minute walk, a swim, gentle yoga, or any movement that gets your body flowing helps move stuck qi and releases the neurochemicals that support mood. The key is consistency rather than intensity.
Sleep. Depression and poor sleep create a vicious cycle. Prioritize sleep hygiene: consistent bedtime before 11pm, no screens for an hour before bed, a cool dark room. Acupuncture improves sleep quality for most patients, which alone can begin to lift depression.
Connection. Isolation is both a symptom and a perpetuator of depression. Even small amounts of genuine human connection can interrupt the downward spiral. This does not mean forcing yourself into social situations that drain you, it means finding even one or two people or activities where you feel safe and present.
Reduce alcohol. Alcohol is a central nervous system depressant. While it may temporarily numb emotional pain, it worsens depression over the medium and long term, disrupts sleep, and interferes with neurotransmitter production. Reducing or eliminating alcohol during depression recovery significantly supports treatment outcomes.
You Do Not Have to Stay Here
Depression lies to you. It tells you that nothing will help, that you have always felt this way, that you always will. That is the depression talking, not reality. Acupuncture offers a path out, not by numbing the pain but by restoring the balance and flow that allow you to feel fully alive again.
If you are in Koh Samui and struggling with depression, book a session at Piraluna. Claire will listen without judgment, identify your pattern, and create a treatment plan that meets you where you are. Taking this step is not weakness. It is the bravest thing you can do.
If you are in crisis, please contact a mental health professional or crisis helpline. Acupuncture is a valuable part of depression treatment, but it is not a substitute for emergency mental health care when safety is a concern.
Can acupuncture help with depression?
Yes. Multiple meta analyses and randomized controlled trials show that acupuncture is effective for treating depression. It increases serotonin, norepinephrine, and dopamine production, reduces neuroinflammation, and regulates the HPA axis. Research shows it is as effective as antidepressant medication for mild to moderate depression and produces better outcomes when used alongside medication for more severe cases.
How many acupuncture sessions are needed for depression?
Most depression treatment courses involve eight to twelve weekly sessions. Many patients notice improvement within the first three to four sessions, with benefits building progressively. Some patients continue with biweekly or monthly maintenance sessions after the initial course. The duration depends on the severity and duration of the depression and the underlying TCM pattern.
Can I use acupuncture while taking antidepressants?
Yes. Acupuncture works safely alongside antidepressant medication and research shows the combination produces better outcomes than medication alone. Acupuncture may also help reduce medication side effects. Never stop or change your medication without consulting your prescribing doctor. Inform both your doctor and your acupuncturist about all treatments you are receiving.
Want the free acupressure guide?
Enter your email and get it delivered instantly.

About Claire
Claire holds both a Bachelor's and Master's degree in Traditional Chinese Medicine from Chengdu University of TCM, one of China's top TCM institutions. With over five years of clinical experience and fluency in Thai, Chinese, and English, she treats patients from more than 20 countries for everything from chronic pain and sleep problems to digestive issues and emotional health.
Learn More →Ready to try acupuncture?
Book a session at Piraluna and feel the difference for yourself.
Book Your SessionContinue reading
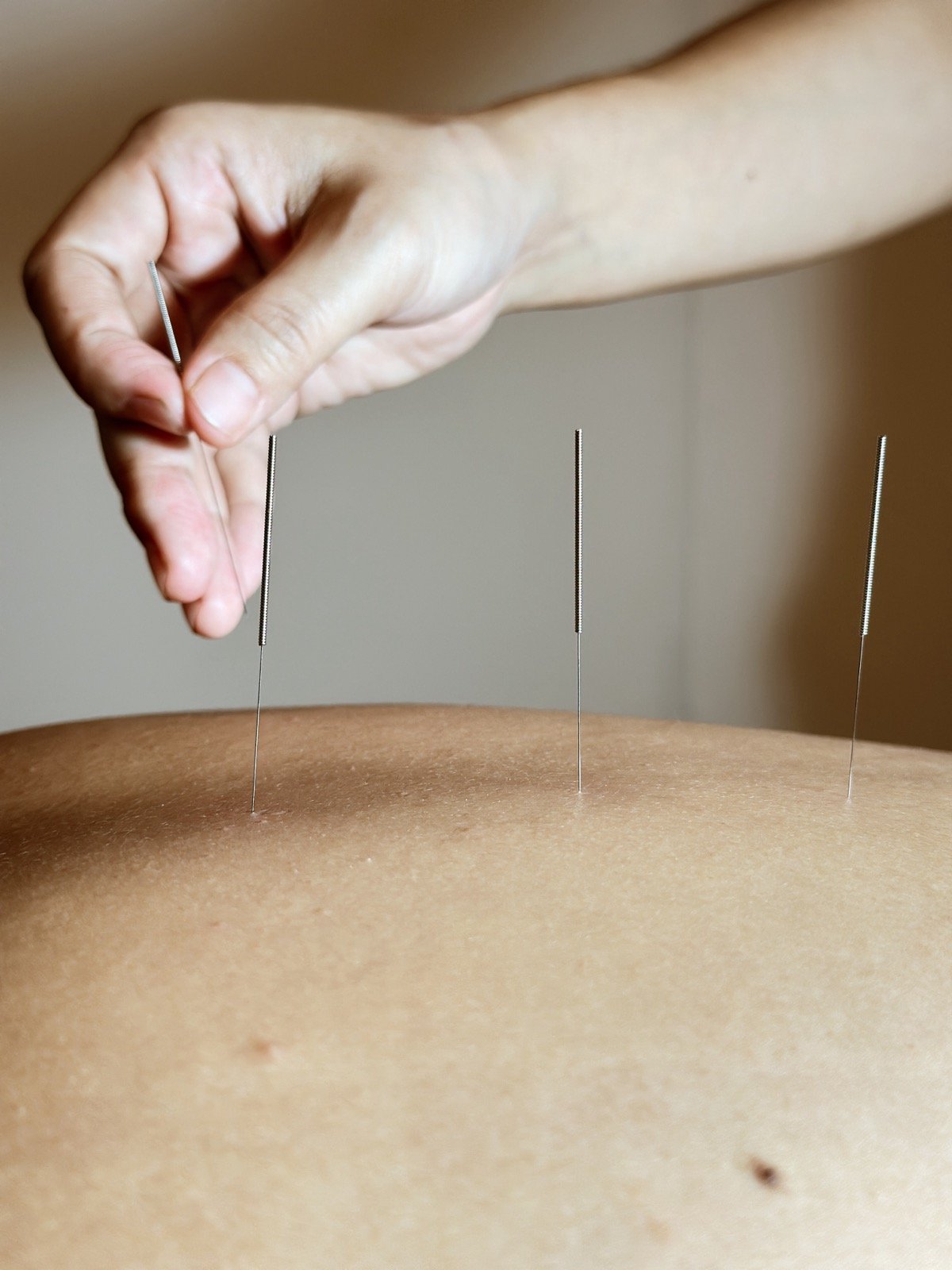
Your First Acupuncture Session: What to Expect
Everything you need to know before your first acupuncture session. What to wear, what the needles feel like, how long it
Read More →
TCM for Women's Hormonal Balance: A Natural Approach That Works with Your Body
How Traditional Chinese Medicine supports women's hormonal balance naturally. Learn about acupuncture for PMS, irregular
Read More →
Acupuncture for Fertility: How TCM Helps You Get Pregnant Naturally
Discover how acupuncture helps you get pregnant naturally. The research behind TCM fertility treatment, what causes infe
Read More →